Bilateral Hippocampal Infarction
- Vernon Williams DO, Colby Jones DO
- Jul 10, 2020
- 6 min read
39M with history of intravenous drug abuse found down • Xray of the Week

Figure 1: Initial MRI of the Brain with and without contrast (hospital day 6) Gyriform increased DWI signal with corresponding decreased ADC signal involving the cortical gray matter of the bilateral hippocampal gyri, compatible with restricted diffusion.
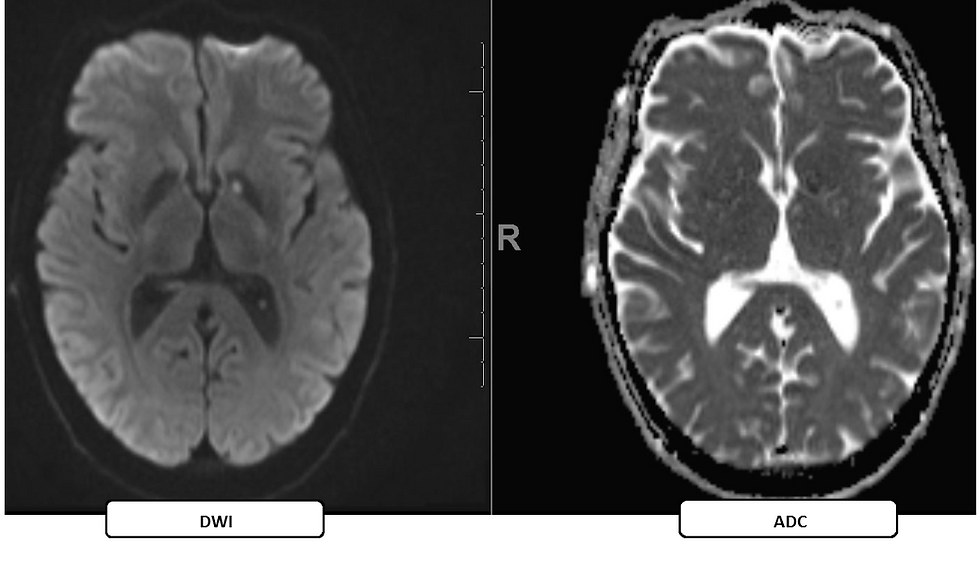
Figure 2: Initial MRI of the Brain with and without contrast (hospital day 6)Within the left globus pallidus is an additional tiny focus of restricted diffusion, representing a lacunar injury.

Figure 3: Initial MRI of the Brain with and without contrast (hospital day 6)Diffuse increased IR/T2 signal involving this region of the bilateral hippocampal gyri, consistent with edema. No involvement of the uncus or other areas of the temporal lobe.

Figure 4: Initial MRI of the Brain with and without contrast (hospital day 6)After administrations of contrast, no significant enhancement is appreciated in either hippocampal region. Subtle tiny focus of enhancement involving the left globus pallidus, corresponding with focus of restricted diffusion.

Figure 5: Follow-up MRI of the Brain with and without contrast (hospital day 16)The hippocampal gyri have diminished volume in the interval and no longer restrict diffusion. There is now bilateral linear peripheral T1 shortening involving the cortical gray matter bilaterally (in the regions of the alveus and fimbria). After administration of gadolinium, subtle patchy areas of enhancement is seen within the hippocampal gyri bilaterally. The previously described punctate focus of restricted diffusion in the left basal ganglia has resolved.

Figure 6: 10-day Interval change between MRI's performed on day 6 to day 16. The hippocampal gyri have diminished volume in the interval and no longer restrict diffusion. There is now bilateral linear peripheral T1 shortening involving the cortical gray matter bilaterally (in the regions of the alveus and fimbria). After administration of gadolinium, subtle patchy areas of enhancement is seen within the hippocampal gyri bilaterally. The previously described punctate focus of restricted diffusion in the left basal ganglia has resolved.
Introduction Isolated bilateral hippocampi injury is a known complication of opioid abuse that is a rare cause of memory impairment or amnesia. The imaging findings, however, overlap with other disease processes and therefore require good clinical history and clinical care to rule out other temporal lobe pathology. This case report aims at discussing the imaging findings of toxic encephalopathy related to hippocampal ischemia.
Case Report Patient is a 39 year-old male, with a past medical history only significant for intravenous drug abuse and recent incarceration, who presented to the ED after being found down on the ground for an unknown amount of time. At presentation, the patient was ill-appearing, in acute distress, hypotensive, and somnolent with GSC of 15. On initial questioning, he reported a recent use of heroin “yesterday” but was otherwise a poor historian with uncertainty of last day of drug use before then.Laboratory analysis was remarkable for a white blood cell count of 30.6 (3.5-10.1 bil/L), C-reactive protein of 39.1 (0.0-7.9 mg/L), creatine kinase of 302,793 (40-230 U/L), potassium of 9.1 (3.5-5.2 mmol/L), and troponins were elevated to 1.19 (0.00-0.03 ng/mL. Initial imaging (CT scans of the head, chest, abdomen, and pelvis) were negative. On hospital day 6 and 16, MRI exams of the brain were performed, which demonstrated isolated bilateral hippocampal infarcts (Figs. 1-6). No evidence of infection was found on a lumbar puncture and blood cultures were negative over the course of his hospital stay. Discussion The etiologies of hippocampal injury include: ischemia, infection, toxic/metabolic, paraneoplastic syndrome, and seizures. Toxic exposure secondary to heroin resulting in ischemia has been described in the medical literature (1). Interestingly, bilateral hippocampal infarction has also been described with acute cocaine intoxication (3). Ischemia is the most common neurovascular complication from opioid abuse (1). A pathologic study on chronic heroin addicts demonstrated gliosis preferentially within the Sommer sector of the hippocampus (CA1 region) (1). It is important to decipher if restricted diffusion in the hippocampus is in an arterial distribution (vascular etiology) vs non-vascular distribution. The hippocampus is located within an end arterial vascular territory and supplied by the anterior, middle, and posterior hippocampal arteries. These arteries create an anastomotic network but during ischemic conditions may lead to infarction. All the remaining etiologies, when seen with bilateral changes, can cause hippocampal dysfunctions such as anterograde amnesia syndromes, but have distinctly different imaging patterns. Limbic encephalitis may present with hippocampal edema with typically no restricted diffusion.
A case report by Marinkovic et al. discussed that sudden memory loss, with prolonged cognitive impairment beyond 10 days was seen with hippocampal stroke in their patient (4). In a case series performed by Bhattacharyya et al. 16 patients with restricted diffusion or bilateral hippocampal lesions were studied. Of the 8 patients with presumed hypoxia, 5 presented with symptoms including confusion and amnesia. All the patients who survived the study had persistent anterograde amnesia ranging from a few days to 20 months, which suggest that the imaging findings regarding the bilateral hippocampal restricted diffusion are significant (2). An additional case series performed by Small et all. concluded that a common link of toxic exposure/substance abuse was present in their 4 patients with acute hippocampal gyriform ischemia. They also believe that these cases may be underestimated due to the nature of treating those with substance abuse and relating the patient’s neurological symptoms (confusion, memory loss) to general acute intoxication. The authors also note that bilateral symmetrical lesions, such as with this entity, may not be readily identified by radiologists which also leads to fewer accurate diagnoses (1). Conclusion Our case illustrates acute ischemia of the bilateral hippocampi as a complication of opioid abuse and as a rare cause for amnesia. The initial MRI of the brain demonstrated acute bilateral hippocampal ischemia. An additional small lacunar injury was seen in the left basal ganglia, further suggesting parenchymal ischemia. Over the course of his hospital stay, no clinical evidence was found for other differential diagnoses. The patients age and negative CT scans of the head, chest, abdomen, and pelvis made paraneoplastic syndrome (limbic encephalitis) unlikely. Negative blood cultures and lumbar punctures excluded underlying infectious process (like herpes simplex virus). The 10-day follow-up MRI of the brain demonstrated laminar necrosis and interval enhancement, evidence of evolving changes related to infarction.
References:
1. Small, J. E., Butler, P. M., Zabar, Y., & Barash, J. A. (2016). Complete, bilateral hippocampal ischemia: a case series. Neurocase, 22(5), 411–415. doi:10.1080/13554794.2016.1213299
2. Bhattacharyya, S., Gholipour, T., Colorado, R. A., & Klein, J. P. (2017). Bilateral Hippocampal Restricted Diffusion: Same Picture Many Causes. Journal of Neuroimaging, 27(3), 300–305. doi:10.1111/jon.12420
3. Connelly, K.L, Chen, X. , Kwan, P.F. (2015). Bilateral hippocampal stroke secondary to acute cocaine intoxication. Oxford Medical Case Reports, March 2015 (issue 3), 215–217. doi:10.1093/omcr/omv016
4. Marinkovic I., Lyytinen J., Valanne L., Niinikuru R., Pekkonen E. Bilateral Hippocampal Infarction as Etiology of Sudden and Prolonged Memory Loss. Case Rep Neurol, 2012(4), 207–211. doi:10.1159/000345564

Vernon F. Williams DO is Diagnostic Radiology resident at Beaumont Hospital, Farmington Hills Campus in Michigan. Prior to residency, he completed undergraduate training at the University of Texas at Austin and Medical school at The University of North Texas Health Science Center, Texas College of Osteopathic Medicine. Dr. Williams will be starting an abdominal imaging fellowship at Vanderbilt University in Tennessee for the academic year of 2020-21. He is a case contributor for the recently published Top 3 Differentials in GI Radiology in 2019.

Colby J. Jones DO is currently a Diagnostic Radiology resident at Beaumont Farmington Hills located in Farmington, MI. Prior to residency, he completed his undergraduate training at Morehead State University, majoring in Biomedical Science. He then completed his 4 years of medical school at the Kentucky College of Osteopathic Medicine. Over the course of his training, he has continued to realize the importance of diagnostic imaging and the direct effect it has on providing care to patients. After completion of his training, Dr. Jones plans to provide quality diagnostic care and support radiological growth in rural and underserved areas.

Rocky Saenz DO FAOCR is currently a practicing Radiologist in Michigan at Beaumont, Farmington Hills, formerly Botsford Hospital. He is the Chairman of the Department of Radiology since 2019. He was Program Director for the Diagnostic Radiology Residency from 2009-2019 at Beaumont Farmington Hills, Botsford Campus, an affiliate of Michigan State University. He completed his first book in 2011, CT for the Non-Radiologist. He was awarded the title of “Fellow” by the American Osteopathic College of Radiology in 2015 (after 10 years of service). He then co-authored a 2nd book in 2015 Neuroradiology Case Review and completed the 2nd edition of CT for the Non-Radiologist in 2016. Dr. Saenz published his latest book in 2019 Top 3 Differentials in GI Radiology. He has published multiple articles in the following journals: American Journal of Roentgenology, Radiology, and Journal of the American Osteopathic College of Radiology and published on-line articles for European Society of Radiology, American College of Radiology, Resident and fellow Section of ACR, and American Journal of Orthopedics. He was awarded, faculty teacher/professor of the year 2019-2020 in the department of Radiology at Botsford Campus.


















Comments